
Buprenorphine/naloxone (Suboxone) and naloxone (Narcan) are effective harm-reduction medications used in the treatment of opioid-related conditions. Due to the rurality of North Dakota, ensuring access to treatment for opioid-related conditions is vital.
Standing orders for naloxone allows medical officers to provide naloxone to individuals aged 18 and older without requiring an individual prescription. Additionally, pharmacists in North Dakota have the authority to prescribe naloxone to individuals at risk of experiencing or witnessing an opioid overdose, further increasing access to this life-saving medication. Taking this into account, the ONE (Opioid and Naloxone Education) Program researchers at NDSU performed an environmental scan of North Dakota pharmacies and healthcare facilities to investigate and compare the accessibility of care for opioid-related conditions from their previous environmental scan performed in 2021.
Among community pharmacies (n=142), 70% had at least one form of buprenorphine/naloxone (brand, generic, or both) available, compared to 62% in 2021. Over 87% (92.3% in rural locations) of pharmacies were prepared to order the medication if a patient had a prescription and 89% of community pharmacies (82.7% rural, 95.5% urban) had naloxone immediately available to dispense. Among telepharmacies (n=13), 30% had any form of buprenorphine/naloxone and over 46% had naloxone available.
Of the total 44 provider locations in North Dakota included in the analysis, rural healthcare facilities accounted for 16 of the analyzed locations, with 7 locations being critical access hospitals and the other 9 locations being clinics or health centers. Roughly 80% of providers were accepting new patients. The average wait time for an appointment was 10 days, ranging from 0-74 days. Providers in urban areas had slightly less availability and longer wait times in 2023 when compared to 2021.
Regarding the geographic distribution of opioid-related treatment, there has not been a meaningful change among the pharmacies or providers since 2021. Compared to the 2021 audit (Figure 1), many of the differences noticed were due to variations in the availability of medications for opioid-related conditions among rural pharmacies. The inclusion of telepharmacy locations in the 2023 audit made a slight improvement in the geographic availability of this aspect. This audit highlights areas for improvement in access to opioid-related treatment within North Dakota. Possible solutions to these areas include expanding telehealth services and increasing collaboration between pharmacies and providers. This research guides public health policy and interventions relating to opioid-related treatment.
Overall, the results of this environmental scan demonstrate North Dakota’s continued progress toward increasing care for opioid-related conditions, albeit at a gradual rate. A map providing a visual representation of BUP/NX treatment availability is below (Figure 2).
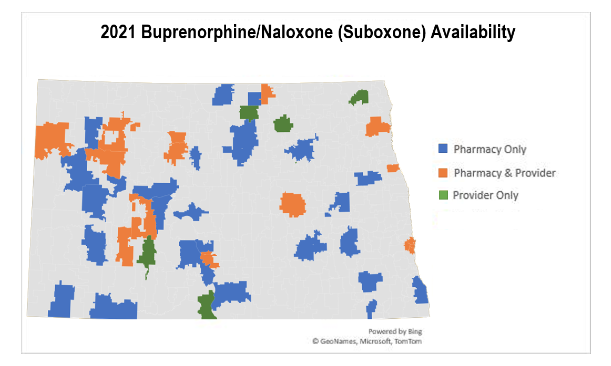
Figure 1 |
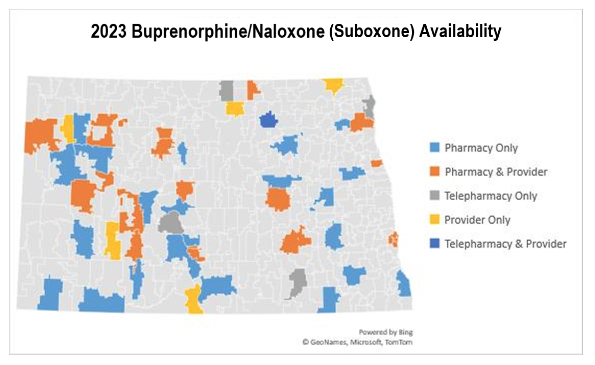
Figure 2 |

The Center for Collaboration and Advancement in Pharmacy (CAP Center) was approved in 2020 to serve as a core for educational, operational, and research capacity for faculty in the College of Health Professions and practitioners throughout the state. The Center prioritizes research which can be feasibly upscaled, impact population health, and be translatable to other settings.
The mission of the CAP Center is to advance patient care and outcomes by providing training, resources, and interventions fostering advancement of pharmacy and collaboration with other healthcare professionals using evidence-based best practices resulting in improved population health outcomes. The CAP Center seeks to develop programs that encompass the four core principles of the Center.
The CAP Center provides students with experiences that will prepare them to work at the top of their professional license upon graduation. The CAP Center provides framework for research efforts in areas of population health management and medication safety.
For questions, contact NDSU.CAPCenter@ndsu.edu.
