Perspectives on “want versus need” vary greatly and are swayed by culture and environment. The concepts of equity versus equality face similar biases. As it relates to healthcare, understanding the difference between social determinants of health, social needs, and social risk factors may help improve health equity.
 “Structural barriers (e.g. governance, policies, culture and societal values) and social and economic factors are at the root of health inequities. If improvements in health are to be achieved, efforts must start there first and always,” explained Sandra Melstad, MPH, public health consultant and founder of SLM Consulting.
“Structural barriers (e.g. governance, policies, culture and societal values) and social and economic factors are at the root of health inequities. If improvements in health are to be achieved, efforts must start there first and always,” explained Sandra Melstad, MPH, public health consultant and founder of SLM Consulting.
As a doctoral candidate at the University of South Dakota School of Health Sciences, Melstad’s dissertation research will explore the capacity of public health professionals to improve health equity in South Dakota communities. Informing workforce development, training and capacity building is the goal for the research project.
Melstad referred to a Health Affairs article on social needs which states, “Until recently, efforts to improve the health of Americans have focused on expanding access to quality medical care. Yet, there is a growing recognition that medical care alone cannot address what actually makes us sick.”
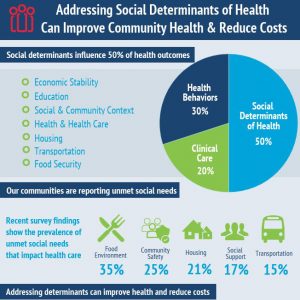 According to data published in October 2019 by the National Institute for Health Care Management Foundation, social determinants influence 50 percent of health outcomes with food insecurities accounting for the highest percent of unmet social needs. Increased use of the emergency department adds to the financial burden, and the study reported people are over two times more likely to go to the emergency room if they struggle with food insecurity, access to reliable transportation or community safety.
According to data published in October 2019 by the National Institute for Health Care Management Foundation, social determinants influence 50 percent of health outcomes with food insecurities accounting for the highest percent of unmet social needs. Increased use of the emergency department adds to the financial burden, and the study reported people are over two times more likely to go to the emergency room if they struggle with food insecurity, access to reliable transportation or community safety.
The article went on to compare individual-level interventions with long-term community solutions, “They (strategies) are often limited to a small segment of the population – those who are in the worst health and have the greatest health care costs. Meanwhile, those patients who do not rank among the ‘sickest and most expensive’ are ignored.”
By facilitating training on health equity practice and collecting data on health disparity populations, Melstad’s work through SLM Consulting is intended to advance health equity by engaging the communities impacted by health disparities and building capacity within the workforce to address health equity.
“These efforts have resulted in improved steps to address health equity in program planning, data collection, and overall integration of a health equity lens in everyday practice.” Melstad summarized the intent of her research effort, “My goal in promoting health equity in public health practice is to make addressing health equity the rule, not the exception, which will improve population health and bridge clinical and community practice to make a sustainable impact.”

