The United States is aging. The number of older adults, individuals ages 65 years and older, is growing rapidly. As we age, care often becomes more complex. Health systems frequently are not prepared for this complexity, and older adults suffer a disproportionate amount of harm while in the care of the health system.
 To address these challenges, The John A. Hartford Foundation and the Institute for Healthcare Improvement (IHI), in partnership with the American Hospital Association (AHA) and the Catholic Health Association of the United States (CHA), set a bold vision to build a social movement so that all care with older adults is age-friendly care, which:
To address these challenges, The John A. Hartford Foundation and the Institute for Healthcare Improvement (IHI), in partnership with the American Hospital Association (AHA) and the Catholic Health Association of the United States (CHA), set a bold vision to build a social movement so that all care with older adults is age-friendly care, which:
♦ Follows an essential set of evidence-based practices;
♦ Causes no harm; and
♦ Aligns with What Matters to the older adult and their family caregivers.
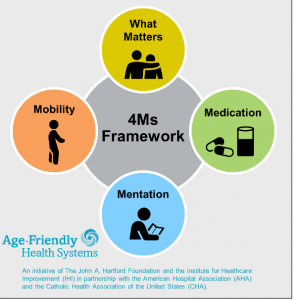
Becoming an Age-Friendly Health System entails reliably providing a set of four evidence-based elements of high-quality care, known as the “4Ms,” to all older adults in your system. When implemented together, the 4Ms represent a broad shift by health systems to focus on the needs of older adults (see Figure to the right).
The 4Ms Framework is an evidence-based model that Great Plains Quality Innovation Network will be using for our Great Plains Quality Care Coalition. The model focuses on four key elements What Matters, Medication, Mentation and Mobility.
What Matters are those specific healthcare concerns, goals and care preferences unique to the individual;
Medications focuses on utilization of only those necessary medications so the individual meets their highest potential in the Ms related to mobility, mentation, and what matters;
Mentation is focused on the prevention, identification, treatment, and management of dementia, depression, and delirium;
Mobility looks to ensure safe mobility, maximum function, so the individual can do what matters to them.
 “These four elements are the essential components of high-quality care for older adults, caregivers and community partnerships. The “4Ms” can be easily understood by patients and families and can be customized for any setting to enhance person-centered care, including vulnerable and rural populations. This cross-cutting framework is being adopted by health systems, stakeholders and organizations across the nation. We look forward to learning more and sharing more details with Coalition members in the coming weeks,” stated Krystal Hays, DNP, RN, CADDCT, CDP, RAC-CT, Hays [pictured] is the Regional Project Manager for the Great Plains Quality Innovation Network.
“These four elements are the essential components of high-quality care for older adults, caregivers and community partnerships. The “4Ms” can be easily understood by patients and families and can be customized for any setting to enhance person-centered care, including vulnerable and rural populations. This cross-cutting framework is being adopted by health systems, stakeholders and organizations across the nation. We look forward to learning more and sharing more details with Coalition members in the coming weeks,” stated Krystal Hays, DNP, RN, CADDCT, CDP, RAC-CT, Hays [pictured] is the Regional Project Manager for the Great Plains Quality Innovation Network.
We are looking for committed nursing homes, hospitals, community leaders, health systems and anyone interested in improving care in your community. Join the Great Plains Quality Care Coalition to:
♦ Partner with an experienced team of quality improvement experts
♦ Access to tools, resources and education
♦ Connect with healthcare partners in your community to share ideas and best practices
♦ Learn how to utilize data to drive improvement
Don’t miss out on this FREE opportunity to be a change maker in YOUR organization and community.
Great Plains Quality Care Coalition. Better Together. Join today!

